Latest News

Important Update 23.03.2026
11.20am - we can confirm the clinical systems running normally now. we will update again should we experience any further issues
As of 10:40am, we are experiencing technical difficulties that are preventing our colleagues from accessing our clinical systems.
This issue has been confirmed as a nationwide problem.
We are continuing to monitor the situation closely and will provide a further update at 11:15am.
Thank you for your patience and understanding.
Patient Communication: MenB Vaccination – University of Kent Students Only
Important information for patients regarding the meningococcal disease outbreak in Kent
As part of the public health response to the recent outbreak of meningococcal disease in Kent, NHS England and UKHSA have advised that some students from the University of Kent may now be eligible for a MenB (Bexsero) vaccination.
Who is eligible?
This vaccination offer is strictly for students from the University of Kent who meet all of the following criteria:
- They have been identified by UKHSA as part of the eligible student cohort
AND - They have not yet received their MenB vaccine at the on‑campus vaccination clinics
AND - They have returned home and are unable to access vaccination at the University of Kent.
If you are not a University of Kent student, you are not eligible for vaccination under this scheme.
Why is this being offered?
UKHSA has confirmed an outbreak linked to Canterbury, with a number of meningococcal group B cases primarily affecting University of Kent students. Vaccination is being offered to a small, targeted group of students to help protect those at increased risk.
If you are eligible
If you are a University of Kent student who has been advised you are eligible and you have returned home, you may contact the practice to request a MenB vaccination.
Please state:
- That you are a University of Kent student
- That you were identified as eligible by UKHSA
- That you were unable to attend the campus vaccination clinic
If you are not eligible
We are unable to offer MenB vaccination to anyone outside the UKHSA-defined University of Kent cohort.
Spring 2026 COVID-19 Booster Vaccination Programme
- Extended Access Clinics: From Monday 13 April 2026
- Saturday Clinics: From Saturday 18 April 2026
- Aged 75 or over, or turning 75 before 30 June 2026
- Aged 18 to 74 and immunocompromised
- Eligible patients will receive an invitation with a booking link on the evening of 17 March 2026
- If you contact the practice, our team will be happy to book your appointment directly
- Our team may also contact you to offer an appointment if you are eligible
Easter Opening Times 2026
The Practice will be closed on the following festive Bank Holidays and open as usual all other dates:
- Good Friday 3rd April
- Easter Monday 6th April
Prescriptions Reminder: Please ensure you order & collect your medication ahead of time
For urgent, but non-life threatening health concerns out of hours, you can access NHS 111 online or by calling 111
For life threatening medical emergencies, such as chest pain or breathlessness, please dial 999
We would like to wish all our patients, their family and friends a Happy Easter
We hope you stay safe & well,
From all the Team at SHP
MSK and Physiotherapy Services for patients
getUbetter App
getUBetter is a self-management app for people with common musculoskeletal injuries or conditions.
getUBetter is a safe and effective way to help you self-manage your injury or condition at home, work, and on the move. The app covers a range of musculoskeletal injuries and conditions.
Self-Refer Physio
You can also now refer yourself directly to the Physiotherapy Service without having to make an appointment to see your G.P. first
Please contact us on one of our central booking lines to make an appointment :
Solihull Community Physiotherapy
TEL : 0121 329 0107
Solihull/Good Hope/Heartlands Physiotherapy Departments
TEL : 0121424 5446
Please note this service is not available for children or for patients with gynaecological, neurological obstetric and respiratory problems and anyone requiring a home visit
Physiotherapy helps to restore movement and function when someone is affected by injury, illness or disability. It can also help to reduce your risk of injury or illness in the future. It takes a holistic approach that involves the patient directly in their own care.
www.nhs.uk/tests-and-treatments/physiotherapy
Nestle recalls several SMA Infant Formula and Follow-On Formula as a precaution because of the possible presence of cereulide (toxin)
Happy Christmas & New Year from the team at SHP
We would like to wish all our patients, their family and friends a Happy Christmas and Healthy 2026!
We hope you stay safe & well,
From all the Team at SHP

Festive Opening Times 2025
The Practice will be closed on the following festive Bank Holidays and open as usual all other dates:
- Christmas Day - 25th December 2025
- Boxing Day - 26th December 2025
- New Year’s Day - 1st January 2026
Prescriptions Reminder: Please ensure you order & collect your medication ahead of time
For urgent, but non-life threatening health concerns out of hours, you can access NHS 111 online or by calling 111
For life threatening medical emergencies, such as chest pain or breathlessness, please dial 999
We would like to wish all our patients, their family and friends a Happy Christmas and Healthy 2026!
We hope you stay safe & well,
From all the Team at SHP

Update on Mask Wearing in Our GP Surgery
Due to a recent rise in flu cases in our local area, our clinicians and reception team will be wearing masks to help protect our patients - especially those who are more vulnerable.
We kindly ask all patients to wear a mask when visiting the surgery site, if you are able to. This small step will help reduce the spread of infection and keeps everyone safe.
If you have any respiratory infection symptoms (e.g. cough, cold, sneezing or flu-like symptoms), please stay at home and call the practice, or call 111 or go online to 111.nhs.uk. Please do not come into the surgery as respiratory infections can spread easily and you could spread the illness to others.
Thank you for your understanding and support.
If you are eligible for a flu vaccination and have not yet had one, please contact the surgery to arrange your vaccination.

A huge THANK YOU to each and every one of our SHP PPG volunteers…
Today (5th December) is International Volunteer Day (IVD), designated by the United Nations in 1985 as a day where volunteers are acknowledged.
This International Volunteer Day we would like to say a huge THANK YOU to each and every one of the volunteers from the SHP Patient Participation Group (SHP PPG), who have supported SHP at the flu vaccination clinics, at our Carers Events and at our various health events, as well as with their vital patient feedback including testing our online consultation platform and new website, to name but a few examples.
Your time and participation as volunteers has made a real difference to SHP, its patients and the local community – Thank you.
Each year, hundreds of millions of people volunteer their time and skills to help make the world a better place - THANK YOU to all volunteers everywhere!

Volunteer members of the PPG get-together on International Volunteers Day
Thank you to all our patients that attended their booked appointments in October 2025
Unfortunately…
1,546
Appointments were not attended in October.
A missed appointment is a loss to the practice and patients like you.
Please support your practice by cancelling an appointment you are unable to make or if it is no longer needed, so it can be offered to someone else.
You can cancel your appointment using the link in the text message, via the NHS App or by calling us and choosing option 2.
Thank you

Armed Forces Veterans Event Success


We are a Veteran Friendly Accredited GP practice

A Reminder - Have you booked your Flu Vaccine yet?
It’s not too late to book your flu vaccine appointment - We have invited all eligible registered patients by text, telephone call or letter to book their flu vaccine appointment.
Are you eligible?
You can get the free #NHS flu vaccine if you:
- are aged 18-64 years old and clinically vulnerable
- are aged 65 or over (including those who will be 65 by 31 March 2026)
- have certain long-term health conditions
- are pregnant
- are the main carer for an older or disabled person, or receive a carer's allowance
- live with someone who has a weakened immune system
How to Book…
If eligible, you will have received an invitation with a self-booking message to book your flu vaccine appointment directly onto one of our flu clinics at Monkspath Surgery, Haslucks Green Medical Centre and Grove Surgery, at weekends and evenings.
You can also book your flu vaccine appointment by calling us on 0121 705 1105 or visiting any of our surgery sites.
If you have a query or wish to decline the flu vaccination and let us know so we can update your records, please email us at nhsbsolicb.shpregistrations@nhs.net
To find out more and if you are eligible for a flu vaccination visit https://www.nhs.uk/vaccinations/flu-vaccine
Stay Strong, Get Vaccinated – Book Today!

Breast Cancer Now's Wear It Pink day is taking place today (24th October 2025).



Happy Pharmacy Technician Day
Its Pharmacy Technician Day today (21st October 2025), and we would like to take this opportunity to thank our Pharmacy Technicians at SHP for all their hard work, compassion and care they provide to our patients.
And if you want to find out what a Pharmacy Technician does, see below ‘A Day in the Life of our Pharmacy Technician’...
A Day in the Life of a Pharmacy Technician at Solihull Healthcare Partnership (SHP)
My name is Kayleigh and I am a Pharmacy Technician here at SHP.
I previously worked as a Pharmacy Technician in Boots after qualifying in 2013, followed by an online pharmacy and then joining Monkspath Surgery in 2016 as a Receptionist. I took on additional training and qualified as a pharmacy technician in 2021 in which I then joined the Pharmacy team.
The most frequent question I am asked is, what is a Pharmacy Technician? Pharmacy Technicians play an important role within general practice and complement the more clinical work of our clinical pharmacists.
Pharmacy Technicians (PTs) are healthcare professionals registered with the General Pharmaceutical Council and in general practice, PTs are supporting pharmacists and GPs to focus on advanced skills by undertaking tasks such as medicines reconciliation on discharge, management of prescription queries and repeat requests, helping patients to get the best from their medicines increasing their compliance and concordance, recommend over-the-counter medication using national guidance, improving repeat prescribing processes, including promotion of repeat dispensing and online ordering, minimising clinical risk and aiming to reduce wasted medicines.
My typical day can be anything from monitoring blood test appointments made for patients on blood thinning medication, to assessing safety alerts from the Medicines and Healthcare products Regulatory Agency (MHRA), to managing a request from an appliance provider who is requesting us to order incontinence products.
I love that every day is different. One minute I can be booking a patient in for a complex medication review with a Pharmacist, the next I can be dealing with a query from a patient checking if their hospital changes for medication have come through and medical record is up-to-date to the next, then I can be contacting a hospital to chase the relevant documents before medication can be prescribed for a patient as requested by one of our Doctors, and then I can be sending out a text message to patients to inform them that if they use steroids that they may need a steroid card. It certainly keeps me busy!
I enjoy the role as you can continue to develop your clinical knowledge and skills (I’m currently doing an asthma course so that I can undertake patient reviews in the future), and I get to have direct contact with our patients. It’s so great to be able to go back to patients and tell them their medication is ready, after they have contacted us to follow up on their medication following a hospital appointment. I like ensuring patients have their medication in time and any changes are done - knowing the patients are happy and that we are helping.

Patient Information - When visiting The Jacey Practice

Online Consultation System
From 1st October 2025, all GP practices are now required to have their online consultation system available throughout core hours for non-urgent appointment requests, medication queries and admin requests.
This brings online access into line with telephone and walk-in, giving parity of access for patients and helping to reduce demand on telephone systems, freeing them up for patients who don’t feel confident to use, or have, digital access.
At Solihull Healthcare Partnership we have already implemented this approach with our new digital system, and the feedback so far shows it is benefitting patients.
A reminder to use our digital online consultation service for non-urgent appointment requests, medication queries and admin requests, which is open during normal practice hours:
Monday–Friday, 8.00am – 6.30pm
For urgent help outside of these hours, use NHS 111 or dial 999 in an emergency.

Do you know your numbers?
High blood pressure is one of the biggest causes of global death.
If left unmanaged, high blood pressure can lead to strokes, heart attacks and other complications.
That’s why it’s important that you know your numbers.
By getting your blood pressure checked and knowing your numbers, you can find out if you have high blood pressure, and then you can take control of your health by making small but significant lifestyle changes and taking medication, if prescribed.
If you’re aged 40 and above, you can get a free blood pressure check at a community pharmacy. Visit the Birmingham and Solihull Integrated Care System website to learn more.

New 24/7 Mental Health Text Service for Birmingham and Solihull
Free, confidential support is now just a text away.
A new, round-the-clock mental health text messaging service has launched, offering immediate support to people of all ages across Birmingham and Solihull. The all-age service is a partnership between Birmingham and Solihull Mental Health NHS Foundation Trust and Shout, the UK’s first 24/7 text support service powered by the charity Mental Health Innovations.
How It Works
Anyone of any age with a mobile phone who is experiencing anxiety, stress, loneliness, depression, or other mental health challenges can text ‘Space’ to 85258 to start a free, confidential conversation with a trained mental health professional.
- 📲 Text ‘Space’ to 85258
- 💬 Receive four quick automated messages
- 🤝 Get connected to a trained mental health professional who will listen, support, and guide you
- 🔒 The service is anonymous, free to use, and won’t appear on your phone bill
No app, registration, or mobile data is required—just a simple text message.
A safe space when you need it most
This new service is designed to be especially helpful for those who may not feel ready to speak on the phone or in person. It offers a discreet, accessible first step toward getting help, whether you're in crisis or just need someone to talk to.
In addition to in-the-moment support, texters can be signposted to a range of local services, including:
- Talking Therapies
- Crisis Cafés
- NHS 111 Option 2
Our Practice Supports Clinical Research
Clinical trials are vital to the future of healthcare, helping find better ways to prevent, diagnose and treat conditions. That's why we are supporting clinical researchers to recruit eligible patients like you.
If you meet the criteria for a study in our area, we'll get in touch to let you know.
To find out more about clinical research and how you can get involved, head to www.patient.info/clinical-research or scan the QR code below.

Solihull Healthcare Partnership - GP Patient Survey 2025 Results*
The latest GP Patient Survey* results were published on the 10th July 2025, and it is pleasing to see that in 2025 Solihull Healthcare Partnership (SHP) has improved on our previous year results, in the following;
- 95% were involved as much as they wanted to be in decisions about their care and treatment during their last general practice appointment
- 95% felt the healthcare professional they saw had all the information they needed about them during their last general practice appointment
- 93% had confidence and trust in the healthcare professional they saw or spoke to during their last general practice appointment
- 90% felt their needs were met during their last general practice appointment
- 85% say the healthcare professional they saw or spoke to was good at treating them with care and concern during their last general practice appointment
- 84% say the healthcare professional they saw or spoke to was good at listening to them during their last general practice appointment
- 75% find the reception and administrative team at this GP practice helpful
- 71% say the healthcare professional they saw or spoke to was good at considering their mental wellbeing during their last general practice appointment
- 70% say they have had enough support from local services or organisations in the last 12 months to help manage their long-term conditions or illnesses
Whilst we are pleased to know we are performing well on some of our GP Patient Survey results, particularly the patient appointment experience, we know we still have more to do to improve the overall experience and access for patients. We are continuing to work hard to implement the recent changes to how patients access care at SHP with the introduction of the Total Triage model and Blix PACO, our new and improved online consultation system.
Following the implementation of our actions to improve access for patients over the past few months, we are already seeing the benefits for patients, including easier access with a reduction in the 8am rush on the telephone and no queues at our surgery sites, and 100% of patient contacts dealt with appropriately by the team, based on clinical need, with no patients asked to call back or directed to NHS 111.
The feedback we have received on the changes to access so far from patients has also been very positive, and we are continuing to actively seek feedback and input from our patients to help us fine-tune the processes and patient experience, to ensure we can meet the needs of our patient population both now and in the future.
As we continuously strive to improve the patient experience, we will be making further changes over the next few months to ensure we continue to improve access, quality and continuity of care, and the patient experience, including launching our new website this summer and further training and development initiatives within the team.
As we implement these changes to benefit patients, we will continue to work with the support and engagement from NHS Birmingham and Solihull ICB, local partner organisations and the SHP Patient Participation Group, to achieve these.
- ENDS -
*GP Patient Survey 2025 results from GP Patient Survey. The GP Patient Survey (GPPS) is an annual England-wide survey about patients’ experiences of their GP practice and is administered by Ipsos on behalf of NHS England. The GP Patient Survey is of patients randomly selected from all GP practices in England and includes questions largely about primary care, but also dentistry and pharmacy. Data for the 2025 survey was collected by online and postal surveys from 30 December 2024 to 01 April 2025, and therefore does not reflect recent improvements in access for patients, however we do see the survey includes important information and provides an opportunity to demonstrate our primary care activity, as well as ensuring we align our improvement plans to meet the needs of patients.
Patient Feedback on the recent changes to how patients access care (09.07.25)
On the 9th June 2025, as part of our commitment to improving the way you access care, we introduced a Total Triage model at the practice, and are already seeing the benefits, including easier access with a reduction in the 8am rush on the telephone and no queues at our surgery sites.
This change came in direct response to patient feedback and since implementing Total Triage we have received positive feedback from you, our registered patients. As we continue to implement this new model we are continuing to actively seek feedback and input from our patients to help us fine-tune the process, and ensure we can meet the needs of our patient population both now and in the future.
Recent examples of patient feedback…

PPG member patient experience using the new Total Triage system –
For further information on the Total Triage model, as well as the latest patient questions and answers, see below.
New Website Testing - Thank you to our Patient Participation Group
We would like to take this opportunity to say a big THANK YOU to the volunteers from our Patient Participation Group (PPG) who have recently taken the time to test our new SHP website and share their feedback with us.
Their invaluable insight will help guide changes we make to ensure the website is user-friendly and easy to navigate for patients.
By listening to our patients, and based on the valuable feedback from our PPG through the draft stage, we have ensured the patient voice is central to the new website.
Thank you once again to the members of the PPG for their time and support, and we look forward to launching our new website this summer.
Solihull Healthcare Partnership Team

Close-up of male hands typing on laptop keyboard indoors.
Patient Update on the Important Changes to How You Access Care at Solihull Healthcare Partnership (27.06.25)
On the 9th June 2025, as part of our commitment to improving the way you access care, we introduced a Total Triage model at the practice, and are already seeing the benefits, including easier access with a reduction in the 8am rush on the telephone and no queues at our surgery sites, and 100% of patient contacts dealt with appropriately by the team, based on clinical need.
Whichever way you contact us, whether it’s using our online form (via our website), by phone or in person at one of our surgery sites, under the Total Triage model, every request for help is being assessed first by our experienced clinical team, ensuring you are directed to the right person, at the right time, in the right place.
This change came in direct response to patient feedback and since implementing Total Triage we have received positive feedback from you, our registered patients. As we continue to implement this new model we are continuing to actively seek feedback and input from our patients to help us fine-tune the process, and ensure we can meet the needs of our patient population both now and in the future.
To view the full ‘Patient Update on the Important Changes to How You Access Care at Solihull Healthcare Partnership’, with an overview of the Total Triage model, the Digital Front Door, patient benefits, key highlights and examples of patient feedback so far, as well as the latest patient questions and answers, click on the link here – Patient Update - Important Changes to How Patients Access Care at Solihull Healthcare Partnership 27.06.25
Important Changes to How You Access Care - Patient Information Session
We recently held a Patient Information Session online where our patients were invited to attend for an update on changes to how to access care at SHP, which was attended by over 280 registered patients, who were all invited to provide their feedback, comments and queries. The patient questions and answers from the session can be found here - Patient Information Session 11.06.25 - Patient Questions & Answers
To see a recording of the session held on the 11th June 2025, please view the video below;
Changes to How You Access Care – Thank you to our patients
We are committed to improving the way you access care and today, Monday 9th June 2025, we introduced a new Total Triage model at the practice, and we’d like to say ‘Thank You’ to all our patients for their support and patience during this transition.
To help us manage this change smoothly and efficiently, we are using Blinx PACO - an online consultation system that supports our team in reviewing requests quickly and consistently. This allows us to direct you to the most suitable healthcare professional and make the best use of our team’s expertise. Blinx PACO has been designed with your feedback in mind, to make accessing our services simpler and more convenient.
The feedback on the new system so far has been very positive, and we have been able to gain insight and valuable feedback from patients.
We would also like to thank both our Patient Participation Group members who supported us this morning at a few of our surgery sites, and those patients who attended the recent patient drop-in sessions we’ve held.
We look forward to you trying the new system!
Thank you.
Important Changes to How You Access Care at Solihull Healthcare Partnership
At Solihull Healthcare Partnership, we are committed to improving the way you access care. From Monday 9th June 2025, we will be introducing a Total Triage model at the practice.
Dr Lad, GP Partner at SHP explains the new Total Triage model at the practice.
Important Changes to How You Access Care at Solihull Healthcare Partnership
At Solihull Healthcare Partnership, we are committed to improving the way you access care. From Monday 9th June 2025, we introduced a Total Triage model at the practice.
This change comes in direct response to patient feedback. We’ve heard your concerns about:
- The daily 8am rush for appointments and the need to move away from a first come first served system
- Long waits on the phone
- Being asked to call back again
- Difficulty in accessing care when you need it most
What is Total Triage?
Under the Total Triage model, every request for help will be assessed first by our experienced clinical team, ensuring you are directed to the right person, at the right time, in the right place. Whether it’s a same-day appointment, a routine review or advice from another member of our team, we will ensure your care is timely, appropriate and effective. It will also enable us to help those patients who struggle to access their healthcare needs and those who require continuity of care.
Whichever way you contact us, our care navigators will not be able to book an appointment when you first contact us. However, our care navigators are trained to support you through the process and we will get back to you once our team have assessed your request.

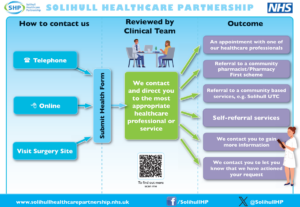
How to contact us
You will continue to contact us in three easy ways:
- Online using a simple form (via our website)
- By phone
- In person at one of our surgery sites
When you get in touch, we will ask you for details about why you’re seeking our help. One of our clinical team will review this information and you’ll receive a response later the same day — this might be a response that we have actioned your request, a call from one of our GPs or Advanced Nurse Practitioners, an appointment with one of our healthcare professionals, advice on the next steps or a referral to another service that better suits your needs.
Why are we doing this
By moving to a Total Triage model, we aim to:
- Eliminate the need to rush for appointments at 8am
- Reduce long waits on the phone
- Ensure vulnerable patients and those with urgent needs get timely care
- Offer routine appointments with continuity, where appropriate
- Prioritise patients based on need, using clinical judgement to prioritise effectively
Supporting this change with Blinx PACO
To help us manage this change smoothly and efficiently, we are using Blinx PACO - an online consultation system, that supports our team in reviewing requests quickly and consistently. This allows us to direct you to the most suitable healthcare professional and make the best use of our team’s expertise.
So what does this mean for patients?
The new system makes it easier for patients to:
- Book or reschedule appointments, avoiding the 8am rush – simply go to our website whenever you need between 8am-6.30pm, Monday to Friday, and submit an online form.
- Provide detailed information about their health concern to our team to get the best healthcare professional service.
- Have more control and flexibility in managing their care.
- Access help with their health without needing to create an account.
- Submit medical and administrative requests from their smart devices (phone, tablet) or computer.
- Access a range of services through one simple online portal.
Other benefits of the new patient experience include…
- Improved access for everyone – by encouraging digital use where possible, we will have more availability on our phone lines for those who need them
- Quick and Efficient - The system allows us to prioritise urgent cases and better manage routine appointments. This should reduce waiting times and ensure patients get timely care.
- Personalised Care – By understanding the patients’ needs upfront, we can direct them to the right healthcare professional at the right time.
- Better Communication – Our team will be better equipped to provide patients with the information and support they need.
We want to hear from you
We have been holding various patient engagement, training and information sessions over the past few weeks with our Patient Experience team, supported by the SHP Patient Participation Group, and on the 11th June 2025 we held an online Patient Information Session where our patients were invited to attend for an update on changes to how to access care at SHP, which was attended by over 280 registered patients who were all invited to provide their feedback, comments and queries.
We have plans for further sessions, both online and in person, over the coming weeks - details and information on how to book your place onto one of these sessions will be sent to our registered patients.
As we continue to implement this new model, we are actively seeking your feedback and input to help us fine-tune the process and make it work for everyone in our community.
Thank you for your continued support as we work to improve access to care and ensure we can meet your needs both now and in the future.
Solihull Healthcare Partnership
FAQs
New Online Service Now live...
A reminder in case you missed it…we’ve been working hard to improve our services based on your feedback, and are pleased to announce our new and improved online service is now live, as we updated our online consultation system from eConsult to Blinx Paco.
On Monday (19th May), we said goodbye to our current online consultation system and transitioned to our new NHS accredited online system. This change means that the forms you are familiar with have been updated and can be accessed via our website.
The new online service ensures;
- We collect the right information first time
- We direct you to the right care pathway from the start
- You receive the most appropriate care for your needs
- Easy access with no account or password needed
- Medical and Admin requests can be submitted
The new online service will help those patient who use digital technology, and also complement those who prefer or need to use our traditional methods of access of visiting us at our surgery sites and by telephone, by enabling us to capture essential information to help direct you to the right healthcare professional or service to fulfil your health needs.
You can access the new version of online forms via our website: https://solihullhealthcarepartnership.nhs.uk
How it works…
Contact us - When you have a healthcare need, simply use our online consultation system. You can use a computer or smart phone to visit our website. If you do not have internet access, then call the practice and our Care Navigators can help you complete the form.
You won’t need to remember a username or password. Instead, you’ll use your NHS number and date of birth to log in. Verification will be done via a code sent to your contact details, simplifying your access to our services.
Locate Your NHS Number – You’ll need this for the new system. You can find your NHS number in your NHS account, NHS App, on any letter from the NHS like a prescription or appointment letter, or through the dedicated service available via the link below;
Visit our website – A reminder you can access the new online system via our website - https://solihullhealthcarepartnership.nhs.uk
Access via our website only: Please note you can only access the new online system via our website – https://solihullhealthcarepartnership.nhs.uk - You cannot access our online system via an App, however we have been made aware by some patients that they have tried to access the new online system via an unofficial App which is asking for their bank details – please note we would never ask you for your bank details or any financial information.


New Online Service Now Live...
A reminder in case you didn’t see it…we’ve been working hard to improve our services based on your feedback, and are pleased to announce our new and improved online service is now live, as we updated our online consultation system from eConsult to Blinx Paco.
The new online service ensures;
- We collect the right information first time
- We direct you to the right care pathway from the start
- You receive the most appropriate care for your needs
- Easy access with no account or password needed
- Medical and Admin requests can be submitted
The new online service will ensure we can collect the right information to enable us to make the right decisions to help you in the most timely and efficient way.
You can access the new online forms via our website: https://solihullhealthcarepartnership.nhs.uk
To find out more visit our website at https://solihullhealthcarepartnership.nhs.uk/latest-news
Thank you for your support, Solihull Healthcare Partnership

Are you ready to Quit Smoking?
Smokefree Solihull are committed to helping you quit smoking for good.
For more information call them on 0121 740 1212 or visit www.smokefreesolihull.co.uk


A Message on behalf of Solihull Healthcare Partnership Patient Participation Group (PPG):

How to access us and ask for help?
We are open and here for you. We are continuing to provide services, and prioritise delivering care and services based on clinical needs.
If you need medical advice or treatment, please call us on 0121 705 1105 or, for non-urgent advice or treatment, visit our website or one of our surgery sites.
By Phone
You can call us on 0121 705 1105. Our telephone lines are open from 8am to 6:30pm, Monday to Friday (excluding Bank Holidays).
You will be asked to first discuss your condition/s over the phone with a trained Care Navigator to assess the most appropriate way to provide your care, which may include a face-to-face consultation, and ensure it is provided by the most appropriate person.
In person
You are able to access us face-to-face by visiting one of our surgery sites to ask in person about booking an appointment, repeat prescription requests and for general queries.
Our sites are open from 8:30am to 6:30pm, Monday to Friday (excluding Bank Holidays):
- Shirley Medical Centre
- The Jacey Practice
- Haslucks Green Medical Centre
- Grove Surgery
- Monkspath Surgery
- Dickens Heath Medical Centre
This ensures we are able to prioritise our focus on patients being able to access us through our telephone system when the demand is at its highest and support improving patient access for the majority of patients.
All sites will continue to be closed on Wednesdays from 12:30pm to 1:30pm, as part of our ongoing staff training and development, which is a priority to ensure we continue to improve service delivery and patient care. We are also dedicated to continuing to further upskill our Care Navigators with a programme of additional training and development to support our clinicians, and to ensure our patients see the right healthcare professionals at the appropriate time.
Our telephone lines remain open throughout the training and in the event of urgent patient needs, we can still be contacted. There is minimal impact on service delivery and no impact on appointments. This time has been chosen to coincide with the period of the day when our Doctors and healthcare professionals are conducting essential face-to-face appointments with housebound patients.
Please be polite and respectful, our GPs and practice teams are available and working hard to support you, your family and friends health and care needs.
Go online
Online services currently provide patients with access to their medical records, repeat medication ordering and COVID-19 vaccination status. Using the service will help you to manage your own health and access healthcare features whenever you need to.
You can visit our web site, and order repeat prescriptions and access your medical records on the NHS App and Patient Access – To access and find out more visit: https://solihullhealthcarepartnership.nhs.uk/online-services/
Our Online Consult facility is currently unavailable for patient safety online and clinical governance reasons. We are in the process of reviewing our online services to improve patient access and services, and will keep patients updated via our web site and social media.
Did you know?
You can visit your local pharmacy (Find a pharmacy - NHS (www.nhs.uk) for clinical advice on minor health concerns.
And for urgent issues or out of hours, you can also call the NHS on 111 or go online to seek NHS advice 111.nhs.uk (NHS 111 online)
Our staff are continuing to work extremely hard to provide services and care, and we would like to thank our patients for your continued support.
#HelpUsHelpYou
